The treatment of heart failure has a specific issue that receives less attention than the illness itself. The problem isn’t that doctors don’t know what to do. The clinical guidelines for managing heart failure with reduced ejection fraction are well-established — there are drug combinations that work, therapies that extend lives, and treatment protocols that cardiologists have spent careers refining. The problem is getting those protocols to the right patient, with the right drug, at the right time, especially when that patient lives two hours from the nearest specialist and relies on a primary care doctor who is managing forty other conditions simultaneously.
That gap is what a research team at Cincinnati’s Christ Hospital set out to close. And the tool they built — a generative AI virtual assistant described by hospital officials as the first of its kind for this specific application — is now showing results that are hard to argue with.
The study, led by Dr. Eliano Navarese, followed two groups of new heart failure patients over twelve weeks. One group had access to the AI virtual assistant; the other didn’t. The group using the AI had better clinical outcomes and fewer hospitalizations. Those two findings alone would be enough to draw attention. But the mechanism behind them is what makes the work genuinely interesting, and worth examining carefully rather than just treating as another headline about technology in medicine.
| Topic | AI Virtual Assistant for Heart Failure Care — Christ Hospital, Cincinnati |
|---|---|
| Institution | The Christ Hospital, Cincinnati, Ohio |
| Lead Researcher | Dr. Eliano Navarese |
| Co-Author / Institute Chair | Dr. Dean Kereiakes — Chairman, Christ Hospital Heart & Vascular Institute |
| AI Tool Type | Generative AI Virtual Assistant (described as first of its kind for heart failure management) |
| Target Condition | Heart Failure with Reduced Ejection Fraction (HFrEF) |
| Study Duration | 12-week follow-up comparing AI-assisted vs. standard care groups |
| Key Outcome | AI group showed better treatment outcomes and fewer hospitalizations |
| U.S. Heart Failure Burden | 6.7 million American adults affected; 450,000+ deaths in 2023 (CDC) |
| Annual Cost | Over $30 billion per year in treatment and hospitalization costs |
| Additional AI Research | Christ Hospital AI tool detected 553/601 confirmed heart attacks vs. 427 by standard care; false positive rate under 8% vs. over 40% |
| Reference Links | WCPO 9 News – AI Technology Helps Detect Severe Heart Attacks, Cincinnati / American College of Cardiology – AI-Enabled Clinician: Heart Failure Advancements |
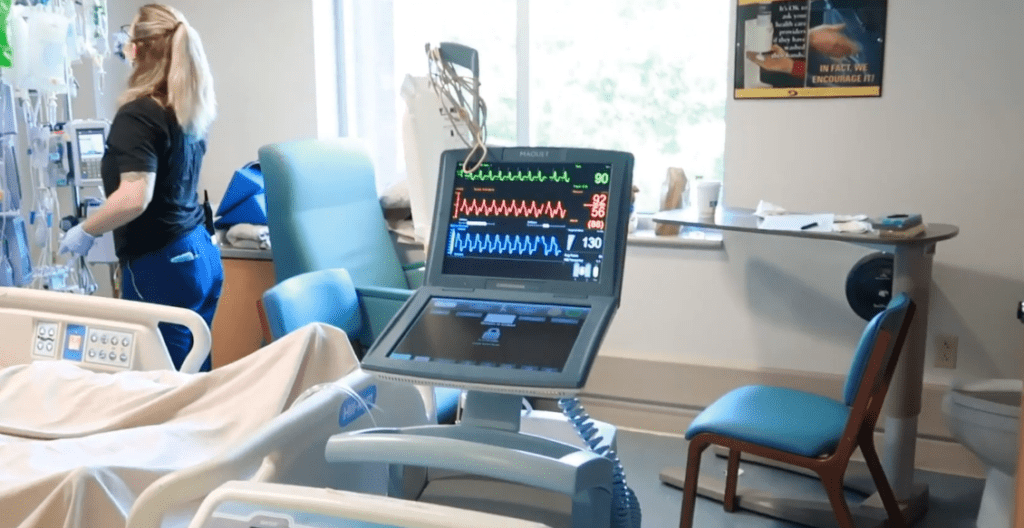
The assistant works by accessing a patient’s existing medical records directly. That means when a primary care physician in a rural clinic needs guidance on treatment — the right medication, the right dosage, the right combination — the AI can generate a recommendation without requiring the doctor to schedule an appointment with an on-call cardiologist, wait for that specialist to review the chart, and then wait again for a callback. The cardiologist still reviews and signs off on the recommendation. But the process is compressed, the friction is reduced, and the patient gets to appropriate treatment faster. Implementation in routine practice has historically been “slow and incomplete because intensive follow-up and specialist time are difficult to scale,” according to the study’s authors’ published findings.” That’s a pretty subdued way of expressing a life-threatening systemic issue.
The value proposition, as stated by Dr. Navarese, is straightforward: the tool instantly gives a primary care provider access to the expertise of specialized doctors. That is not an exaggeration. This system is attempting to address the particular issue that has long been absent from underserved and rural cardiac care. The study’s co-author, Dr. Dean Kereiakes, chairman of Christ Hospital’s Heart & Vascular Institute, directly supported the clinical reasoning, pointing out that the AI assistant adheres to the same rules as human doctors—it is not creating new medication, but rather more effectively administering existing medication.
Perhaps this work’s most important implication has nothing to do with Cincinnati. Christ Hospital is an urban facility with ample resources. The patients who stand to benefit most from a system like this are the ones in places that don’t have a Christ Hospital nearby — rural communities where a cardiologist visit might mean a half-day round trip, where follow-up care after a heart failure diagnosis is inconsistent at best, and where the gap between what guidelines recommend and what patients actually receive is widest. The CDC’s numbers on heart failure make the scale of this problem concrete: 6.7 million American adults are living with the condition, more than 450,000 died from it in 2023, and the annual cost of treatment and hospitalization exceeds $30 billion. When applied to that population, even slight improvements in care delivery yield significant results.
Christ Hospital’s AI efforts are not isolated. Separately, a related study from the same institution discovered that an AI tool analyzing EKG data could remarkably accurately identify severe heart attacks, or STEMI events, where a coronary artery is completely blocked and minutes are truly life-or-death. Over 1,000 patients from three hospitals over a four-year period were examined in that study. The AI identified 553 out of 601 confirmed heart attacks; standard care caught 427. With AI-assisted reading, the false positive rate decreased from more than 40% with traditional methods to less than 8%. The research’s principal investigator, Dr. Timothy Henry, who also oversees Christ Hospital’s Carl and Edyth Linder Research Center, highlighted the tool’s unique usefulness with complicated EKG presentations—the STEMI mimics that even seasoned medical professionals occasionally misinterpret. The AI provided a 95% chance of a correct diagnosis in those situations.
As this corpus of work grows, there’s a sense that the application of AI in clinical medicine is changing in a significant way. The earlier wave of health AI — the diagnostic algorithms trained on clean datasets, the products that performed beautifully on benchmarks and struggled in real-world settings — generated a lot of skepticism that was, in many cases, earned. What’s different about the Christ Hospital work is its grounding in a specific, stubborn, well-documented problem: the inability to deliver specialist-level cardiac care at the pace and scale that patients need. The cardiologist is not being replaced by the AI. It’s trying to make the cardiologist’s knowledge accessible in rooms where no cardiologist is standing.
It’s still unclear how quickly this kind of system can move toward broader adoption, or what regulatory pathways will look like as generative AI tools become more embedded in clinical workflows. For some of these technologies, the FDA piece is still pending, and the issue of liability when an AI recommendation results in a less-than-ideal outcome is still extremely complex. However, the outcomes are quantifiable, the 12-week study results are published, and the hospitals conducting these trials are not marginal academic outposts. These are local establishments that treat actual patients while keeping an eye on their numbers. At least that part is no longer speculative.
